Understand Alzheimer’s and dementia?
Alzheimer’s disease is a progressive neurodegenerative disorder that primarily affects cognitive function, memory, and behavior. It is the most common cause of dementia, accounting for approximately 60-80% of cases. Named after Dr. Alois Alzheimer, who first described the condition in 1906, Alzheimer’s disease is characterized by the gradual degeneration and loss of neurons in the brain, leading to a decline in cognitive abilities and functional independence.
Key features of Alzheimer’s disease include:
- Memory Loss: One of the hallmark symptoms of Alzheimer’s disease is the impairment of short-term and long-term memory. Individuals may have difficulty remembering recent events, recalling familiar information, and learning new information.
- Cognitive Decline: Alzheimer’s disease progressively affects various cognitive functions, including language, problem-solving, attention, and executive function. As the disease advances, individuals may experience difficulty with communication, reasoning, and decision-making.
- Behavioral and Psychological Symptoms: Alzheimer’s disease can also lead to changes in behavior and mood. Individuals may exhibit symptoms such as agitation, irritability, anxiety, depression, and apathy. These behavioral changes can significantly impact quality of life for both patients and caregivers.
- Functional Impairment: As Alzheimer’s disease progresses, individuals may experience difficulties performing activities of daily living independently. Tasks such as dressing, bathing, grooming, and managing finances may become increasingly challenging and eventually require assistance from caregivers.
- Neuropathological Features: The characteristic neuropathological hallmarks of Alzheimer’s disease include the accumulation of abnormal protein aggregates in the brain. These include beta-amyloid plaques, which form extracellularly, and tau tangles, which form intracellularly. These protein aggregates disrupt neuronal function and contribute to neuronal death and brain atrophy.
- Progressive Nature: Alzheimer’s disease is progressive, meaning that symptoms worsen over time. The rate of progression varies from person to person, but in general, individuals with Alzheimer’s disease experience a gradual decline in cognitive function and functional abilities, leading to increasing dependence on others for care.
- Risk Factors: While the exact cause of Alzheimer’s disease remains unknown, several risk factors have been identified, including age, genetics (e.g., presence of certain gene variants such as the APOE ε4 allele), family history of the disease, and certain lifestyle factors (e.g., cardiovascular health, physical activity, and cognitive engagement).
Currently, there is no cure for Alzheimer’s disease, and available treatments primarily focus on managing symptoms and enhancing quality of life for those affected. The medical community continues to research and develop potential disease-modifying therapies that aim to target the underlying pathological mechanisms of Alzheimer’s. These efforts include the pursuit of drugs that can slow or perhaps even halt the progression of the disease, a breakthrough that could significantly alter the treatment landscape.
Early diagnosis is crucial in the management of Alzheimer’s disease as it allows for the timely planning of care strategies and implementation of treatments that can help manage the more debilitating symptoms of the disease. Comprehensive care planning and robust support systems for both patients and their caregivers are key components in coping with the day-to-day challenges of Alzheimer’s. These measures not only help in managing the disease but also in maintaining the best possible quality of life for patients.
Engagement in a supportive community and access to dedicated healthcare professionals can provide the necessary guidance and emotional support for families navigating the complexities of Alzheimer’s care. This holistic approach is vital for both managing the disease effectively and improving the overall well-being of both patients and their caregivers.
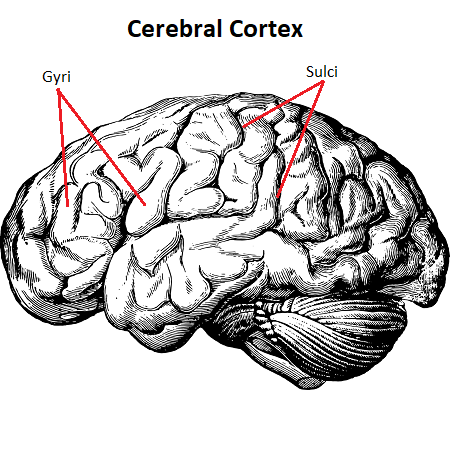
It is important to clarify the difference between dementia and Alzheimer’s as both are commonly mistaken to be the same as the other. Dementia is an umbrella term for the general decline in memory, reasoning or other forms of thinking, while Alzheimer’s is a brain disease that demonstrates symptoms of dementia in its patients. Alzheimer’s is a brain disorder that slowly decays the memory and thinking skills of its victims and also influences their behavior and personality. Because of these symptoms, scientists have determined that Alzheimer’s particularly targets the hippocampus in the brain, as it is responsible for memory encoding and consolidation. However, as time goes by, the decay spreads to other areas of the cerebral cortex. The cerebral cortex is the surface layer of the brain, and holds many important tasks such as language, reasoning, thought, learning and other aspects of higher-level thinking.
We know what Alzheimer’s is capable of doing, but how does this affect the patient’s life and what are some noticeable differences throughout the various stages of Alzheimer’s?
In Stage 1 of Alzheimer’s (also referred to as the normal stage), there is no visible change in the victim’s behavior nor is there any damage to their memory or reasoning, hence why those in this stage are also known as mentally healthy people.
In Stage 2, the patient normally says that they cannot remember things as easily as they used to, and while it is some form of memory loss, it is relatively common in those over 65 to not remember things as easily, hence the coined term cognitive decline can be applied here.
In stage 3, the symptoms of Alzheimer’s begin to manifest and actively affect the victim. They begin to learn significantly slower or begin to repeat questions and perform functions with more difficulty. At this point, the decaying of the cerebral cortex has begun and is negatively impacting the brain’s cognitive functions; but, most of the symptoms are subtle, so families or close ones of the people in this stage likely don’t notice until the end where its effects become much more visible.
In stage 4, the symptoms of dementia become more prevalent and at this point, patients are diagnosed with mild dementia and begin to lose memories about important events in their lives and tend to have difficulties living independently at this point. Now, a diagnosis for Alzheimer’s can easily be made without any medical equipment due to the severity of memory loss being incomparable to that of cognitive decline. c
In Stage 5, the person cannot live independently and tends to have difficulties in decision-making regarding clothes and food, and their memory loss typically causes them to forget important aspects of their current life such as their address or phone number, but this stage does not last particularly long, only about a year and a half on average.
In Stage 6 is where severe cognitive decline is noted and typically displays moderately severe dementia, although stage 6 itself has 5 different substages. In general though, most of these stages display problems in toiletry, clothing, and bathing, but their cognitive deterioration may reach the point where they confuse their closed ones with each other, or they are unable to do basic calculations, and begin having breakdowns in their speech. But most notably, they begin to have emotional breakdowns and a fear of being left alone (because of their reliance on other people).
In the final stage, Stage 7, the patient begins to absolutely require assistance in basic life, and experiences severe declines in speech and ability to walk, and if they are still alive, they are unable to sit up straight in chairs. And then they begin to lose the ability to make facial expressions, now resting at a grimace, and after that they lose the ability to hold their head up. After this point, the person can technically survive indefinitely, but during stage 7, most patients tend to succumb due to other causes, with the most prominent being pneumonia.
Currently, there is no cure for Alzheimer’s, however, there are several medicines that are used to treat the symptoms of Alzheimers and cope with the behavioral consequences resulting from the disease. Currently, a medication known as aducanumab is being used to treat some symptoms of Alzheimer’s, reducing amyloid deposits in the brain which generates at an accelerated pace due to Alzheimer’s. Alzheimer’s tends to break down a neurotransmitter known as acetylcholine, which is a necessary chemical for memory and thinking. So, to counter this, scientists use cholinesterase inhibitors as treatment, due to its ability to prevent the breakdown of acetylcholine, however, because Alzheimer’s also prevents the production of acetylcholine as time progresses, these drugs would eventually become useless as time goes on. For severe and moderate Alzheimer’s, different medications are employed for treatment. One such medication is memantine, which helps people continue daily tasks without assistance (but only for a small while). It does this by regulating the excessive production of glutamate, which prevents cell death in the brain. Furthermore, some medicines are used (with caution) to treat the behavioral effects of Alzheimer’s, for example, anti-anxiety to prevent agitation in patients; anticonvulsants to treat aggression; antipsychotics to treat paranoia and hallucinations. But, these drugs contain several nasty side effects that could result in further risk to the patients, hence why studies are conducted to research for safer, alternative medicines that can treat Alzheimer’s and its behavioral consequences.
![]()
Discover more from Shaivam Kale
Subscribe to get the latest posts to your email.